'Chemo Bath' Being Used To Target Difficult To Treat Cancers In Abdomen
Follow KDKA-TV: Facebook | Twitter
PITTSBURGH (KDKA) - When cancer forms in places like the abdomen, it can be hard to target the treatment. But, there is an approach that can fight it.
Gevony Williams was in her first trimester of pregnancy when she developed a low pain in her belly. It turned out to be a ruptured appendix.
After surgery, she went for her follow-up visit.
"I thought he was just going to be like, you're Superwoman, you've healed so well, you're doing great," she says, "and instead he told me, you know, I need to talk to you, can you sit down for a second?"
She had cancer -- a rare type called goblet cell carcinoid -- and it had spread from her appendix to nearby organs in her belly. Immediately, a team of doctors assembled to take care of her.
"They immediately understood that they weren't just taking care of me, they were taking care of my son, as well, and we had to make some pretty big decisions," Gevony says.
Terminating the pregnancy was not an option.
"We tried for years to get pregnant," she says.
The team got Easton to 32 weeks, and he was delivered by C-section. Gevony bonded with her newborn for two weeks in the NICU at West Penn Hospital.
Then, she was taken to Allegheny General Hospital for treatment of her cancer.
She was a good candidate for a chemo bath -- hyperthermic intraperitoneal chemotherapy -- or HIPEC. It is for a number of cancers within the abdomen.
"When you go with HIPEC, you're actually putting the chemotherapy directly on the cancer cells," explains Allegheny Health Network cancer surgeon Dr. Thomas Krivak.
"It was first pioneered in the mid-1990s," adds AHN cancer surgeon Dr. Suzanne Schiffman.
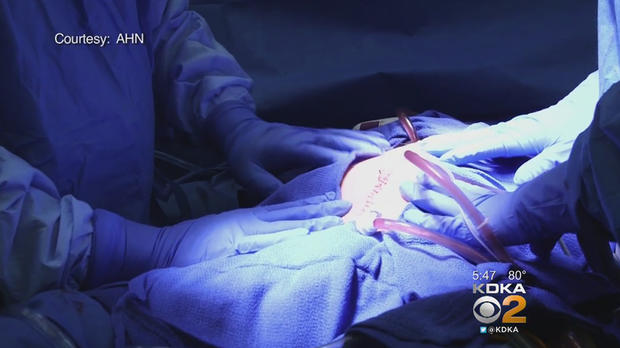
The doctors surgically open the belly, remove all the tumor they can see, and then put the chemotherapy medicine directly into the abdominal cavity. It is heated to improve penetration and its cancer-killing ability. The idea is to treat microscopic disease millimeters deep into the tissues.
"I was physically rocked by medical students so that the solution got all around my abdominal cavity," says Gevony. "It had to remain in there for about 90 to 100 minutes."
"At the end, we drain it all out, and then we do irrigate it out," says Dr. Schiffman.
Dr. Krivak says the ideal patient is physically fit. It is an aggressive surgery, lasting six to eight hours. There is a risk of stroke, heart attack, need for transfusion, and poor wound healing. There is a lot of pain afterwards, and sometimes a bag on the skin for an ostomy -- a rerouting of the intestines to the outside.
"I always tell them they have a higher risk of numerous complications," says Dr. Krivak.
Patients will typically get chemotherapy by vein later.
Gevony had a long and tough recovery, but it was worth it.
"I'm cancer free, I have to be closely monitored and seen pretty regularly amongst my team of doctors," she said.
"She was and her baby were the most important and the system went around to make sure even in this time of having cancer that she got to have that great experience with her baby," says Dr. Krivak.
"I have so much to look forward to. I feel so much better, and just every day is a blessing, really. I'm just trying to enjoy my baby now," says Gevony. "I don't want my son to have memories of a sick mom. And I definitely want to be here for him."